Bioscience
Studying the genes behind surplus X chromosomes
Stem cell analyses could reveal how extra doses of some genes lead to the characteristics seen in males born with one or more surplus X chromosomes.

One in every 500 to 1,000 males are born with one or more extra X chromosomes, leading to a wide range of progressing symptoms with each extra chromosome, including infertility, enlarged breasts, osteoporosis, diabetes, heart abnormalities, intellectual disability and cancer. Now, KAUST scientists have used stem cells, reprogrammed from people with this condition, to improve understanding of how it develops.
People born as males typically have one X and one Y chromosome, whereas females have two X chromosomes. One of the two X chromosomes in females is usually inactivated, except for a small number of “escape” genes. X inactivation also happens in males born with one (Klinefelter syndrome) or more (higher grade sex chromosome aneuploidies, or HGAs) extra X chromosomes. But this still leaves the extra escape genes.
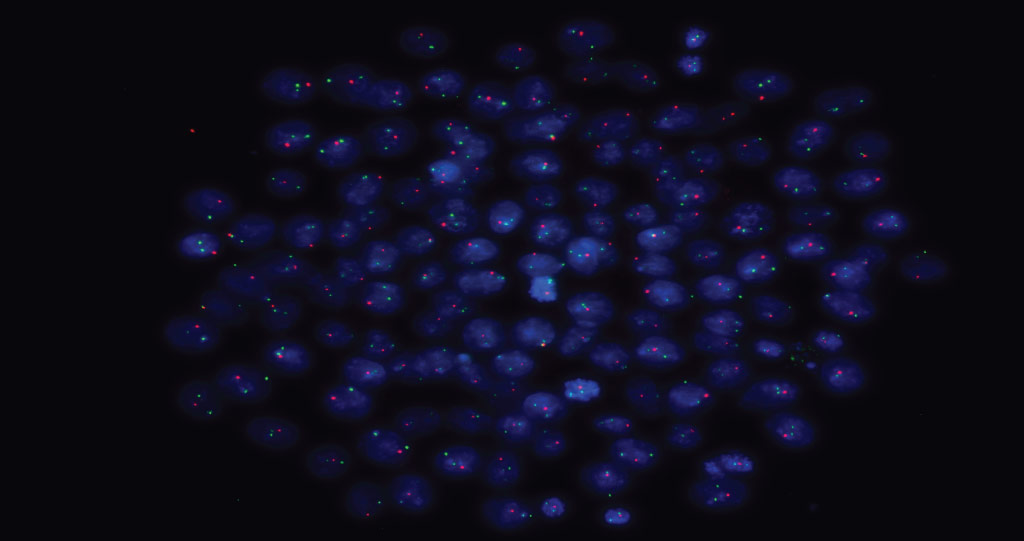
This cell image shows a DNA FISH of an induced pluripotent stem cell (IPSC) colony obtained from a Klinefelter patient stained for X(green) and Y (red) chromosomes in the nuclei (blue).
© 2022 KAUST; Elisabetta Fiacco.
“Scientists have never focused on which genes are responsible for the plethora of features in Klinefelter syndrome and HGAs,” says research scientist Veronica Astro.
“We generated the largest cohort of induced pluripotent stem cells derived from patient fibroblasts to study the effects of having extra copies of the X chromosome in males,” explains Astro. “We also took advantage of KAUST’s cutting-edge technologies to compare gene expression between these and healthy stem cells to identify the genes that are aberrantly expressed in this genetic condition.”
The researchers showed most escape genes were found in a region of the short arm of the X chromosome called pseudo-autosomal region 1 (PAR1). Eleven were linked to progressive severity of symptoms with each extra X chromosome. These genes largely remained active when the researchers programmed the stem cells to develop into pre-liver and pre-pancreas cells. Their activity was dosage-sensitive: it increased with an increasing number of X chromosomes in the cells.
To further test their stem cells, the researchers also examined differences in gene regulators called transcription factors and found that a protein called nuclear respiratory factor 1 (NRF1) was overexpressed in the stem cells with extra X chromosomes, with impacts on a gene called zinc finger protein X-linked (ZFX).
“Importantly, we generated the first ever described cellular platform of induced pluripotent stem cells with various degrees of X chromosome aneuploidies that can be exploited to study the consequences of gene overdosage in early embryogenesis,” says bioscientist Antonio Adamo, who led the study.
Further efforts should help reveal the mechanisms behind the characteristics seen in people with Klinefelter syndrome and HGAs. The stem cell platform could also be used to screen drugs for treating these conditions.
Adamo’s team are now differentiating induced pluripotent stem cells with varying degrees of X chromosome aneuploidies into disease-relevant cell types — like nerve, heart, pancreas and sperm cells — to study how extra X chromosomes impact different tissues.
References
-
Astro, V., Alowaysi, M., Fiacco, E., Saera-Vila, A., Cardona-Londono, K. J., Cigliano, R.A. & Adamo, A. Pseudoautosomal region 1 overdosage affects the global transcriptome in iPSCs from patients with Klinefelter syndrome and high-grade X chromosome aneuploidies. Frontiers in Cell and Developmental Biology 9, 801597 (2022).| article
You might also like
Bioscience
Single small-molecule model reveals insights into human embryo development

Bioscience
Can AI finally bring order to biology’s data deluge?

Bioengineering
Bio-inspired network structures for next-generation AI

Bioscience
Robust workflow built for chemical genomic screening

Bioscience
Cell atlas offers clues to how childhood leukemia takes hold

Bioscience
Hidden flexibility in plant communication revealed

Bioscience
Harnessing the unintended epigenetic side effects of genome editing
Bioscience




