Electrical Engineering
Gentle sensors for diagnosing brain disorders
New sensor design paves the way for safer and more effective brain monitoring.
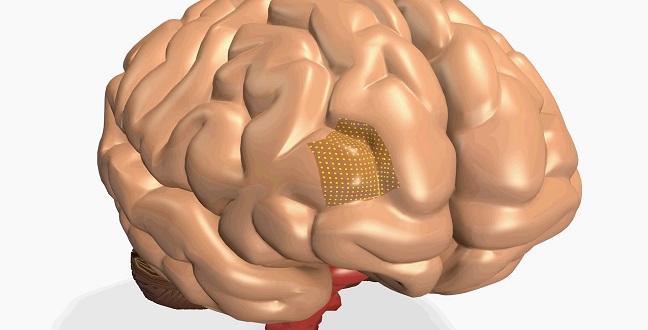
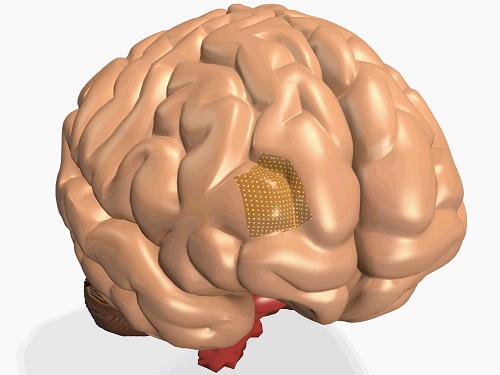
Polymer Vias-based 3-D integration simplifies the path towards high-resolution brain machine interfaces.
© 2016 KAUST
Flexible, low-cost sensor technology leading to safer and improved diagnoses and treatment of brain disorders has been developed by KAUST scientists1.
Mapping the electrical activity of the brain is critical in understanding neurological disorders like depression and Alzheimer’s disease. Multielectrode arrays called Michigan or Utah arrays are currently used to monitor brain activity. Made from layers of conductive silicon needles, these rigid devices are inserted through the scalp to monitor the brain’s surface. The needles can cause inflammation of the tissues, so they must be removed within a year.
Muhammad Hussain and Aftab Hussain from the Computer, Electrical and Mathematical Science and Engineering Division wanted to develop a soft and flexible sensor that could be placed on the surface of the brain within the intracranial space, providing better contact and reducing the risk of damage to tissues.
“Sensors require associated electronics to interface with us, and these electronics dissipate heat, thereby causing a burning effect in the brain that can permanently damage tissues,” explained Muhammad Hussain. “The challenge is to keep the electronics away from the brain.”
Working within these parameters, they fabricated a sensor made from gold electrodes encased in a polymer coating with the connections oriented vertically, and, by placing the connectors on top of the sensor and allowing them to pass through the polymer support, an integrated circuit (IC) could be attached to the flip side of the device, isolating it from the brain surface and preventing hotspots.
The intracranial space of the brain presents an area of only 64 cm2 for mapping more than 80 billion neurons, so not only is it safer to prevent the electronics from making contact with the brain, but it also maximizes the number of neurons that can be monitored by the sensor array.
“The sensor is in contact with the soft tissues of the brain where it collects activity data, and the IC is placed on top, with a soft insulating polymeric material separating them, allowing a larger area to be mapped and a reduction in the heating effect,” Hussain noted.
By using state-of-the-art technology used for fabricating integrated circuits, the researchers developed a method that could lead to mass-produced sensors that are safer, have improved mapping capabilities and are also robust enough for long-lasting functionality.
“We are currently collaborating with Harvard-MIT Medical Institute on using the technique to improve the efficiency of the mapping interface system,” Hussain said.
References
- Hussain, A.M. and Hussain, M.M. Deterministic integration of out-of-plane sensor arrays for flexible electronic applications. Small, 25 July 2016 (doi: 10.1002/smll.201600952).| article
You might also like

Computer Science
AI-based hydrogen plant models improve power grid stability

Electrical Engineering
Quantum dot lasers outshine expectations

Bioengineering
Self-aware biosensors boost digital health monitoring

Bioengineering
Smart patch detects allergies before symptoms strike

Computer Science
Green quantum computing takes to the skies

Electrical Engineering
Micro-LEDs boost random number generation

Bioengineering
Sensing stress to keep plants safe

Computer Science



